Key Takeaways
- Skin infections can range from mild irritations to severe conditions requiring urgent care.
- Common signs include redness, swelling, pain, itching, pus, or fever.
- Risk increases with broken skin, weakened immunity, diabetes, or poor hygiene.
- Prompt medical care, including doctor-recommended antibiotics, antifungals, or antivirals, prevents complications.
- Exceptional Emergency Centers have emergency rooms in Livingston, Beaumont, and Tyler for urgent skin infection care.
What Are Skin Infections?
Skin infections occur when harmful microbes breach the skin’s natural barrier, triggering inflammation and tissue damage. These infections may be bacterial, viral, fungal, or parasitic, affecting either surface or deeper layers of skin. A survey of 878 people in rural Nepal found 62.2% had skin diseases, with infectious conditions like fungal, bacterial, and parasitic infections being most common.
Symptoms Of Skin Infection
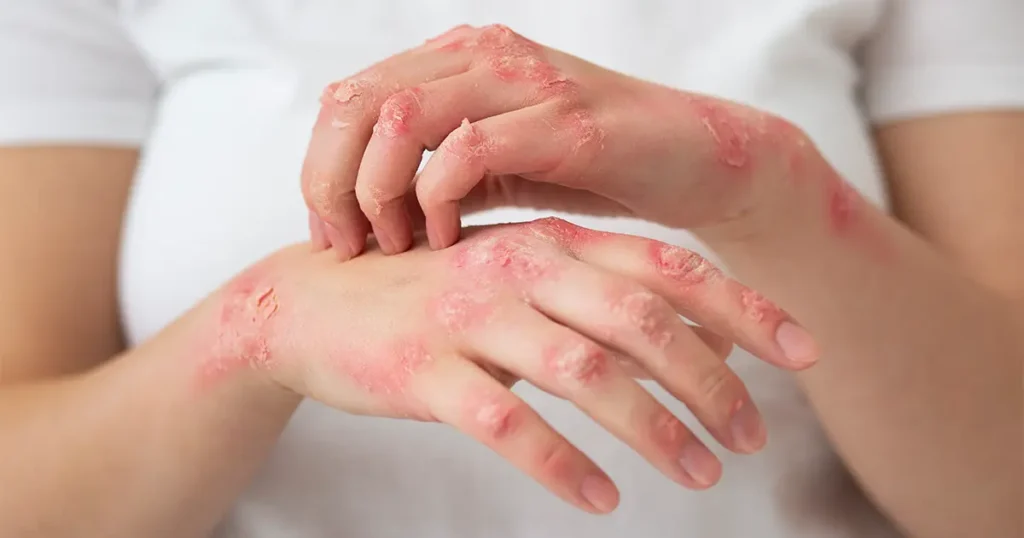
- Redness and Inflammation: The infected area often becomes warm, red, and swollen as the immune system responds.
- Pain And Tenderness: Pain may occur, especially when touched, indicating deeper involvement.
- Pus Or Drainage: Thick yellowish or greenish fluid is a classic sign of bacterial infection needing medical treatment.
- Itching Or Rash: Common in fungal and parasitic infections like ringworm or scabies.
- Fever Or Systemic Symptoms: Fever, chills, or swollen lymph nodes suggest the infection may be spreading.
Types Of Skin Infections
Skin infections can be bacterial, fungal, viral, or parasitic. Severity varies, but all disrupt the skin’s protective barrier. Proper identification and timely treatment are key to avoiding complications.
- Bacterial Infections: Cellulitis, impetigo, erysipelas, often painful, swollen areas that may ooze pus.
- Fungal Infections: Athlete’s foot, ringworm, itchy, scaly rashes in warm, moist areas.
- Viral Infections: Shingles, cold sores, blisters caused by viral replication in skin cells.
- Parasitic Infections: Scabies and lice, mites, or parasites causing itching and irritation.
What Causes Skin Infections?
Skin infections occur when pathogens overcome the skin’s natural defenses. Breaks in the skin, weakened immunity, warm or moist environments, and close contact with infected individuals all increase risk. Preventive hygiene, proper wound care, and early medical evaluation are crucial.
1. Bacteria
Bacteria enter through cuts, scrapes, or surgical wounds, triggering redness, swelling, and pus. Doctor-recommended antibiotics help stop infection progression and prevent systemic complications. Bacterial colonization can also lead to changes in skin texture and the formation of pustules or abscesses.
2. Fungi
Fungi flourish in damp, warm areas, causing rashes, scaling, and itching. Topical or oral antifungals prescribed by a physician clear the infection and reduce recurrence risk. Fungal infections often cause peeling, cracking, or discoloration of the affected skin, particularly in folds or between toes.
3. Viruses
Viral infections like shingles or herpes simplex invade skin cells, producing blisters or sores. Antiviral medications prescribed by healthcare providers help reduce symptoms and prevent the spread. Viral skin infections frequently create vesicles or crusted lesions that follow nerve lines or localized skin areas.
4. Parasites
Parasitic infections, such as scabies mites, burrow into the skin, causing itching and rash. Close contact facilitates spread, but topical doctor-recommended treatments are effective. These infections often result in small, raised bumps, burrow tracks, or intense redness on the skin surface.
5. Breaks In Skin
Cuts, scrapes, or wounds can allow microbes to enter, increasing infection risk. Proper cleaning, bandaging, and medical care prevent severe infection and complications. Even minor skin breaks can alter the skin’s barrier function, making the area more prone to inflammation and localized irritation.
6. Weakened Immune System
Individuals with diabetes, HIV, or other conditions may have reduced immunity, making infections more severe. Timely treatment and monitoring reduce risks. Reduced immune response can lead to slower healing and prolonged inflammation, making the skin appear pale, dry, or more susceptible to lesions.
Who Is Most At Risk For Skin Infections?
Certain groups are more vulnerable due to age, medical conditions, or lifestyle. Awareness and preventive measures are essential.
- Older Adults: Aging skin is thinner and more prone to tears.
- Diabetes Patients: Poor circulation increases susceptibility.
- Immunocompromised Individuals: Weakened immunity heightens infection risk.
- People With Skin Conditions: Eczema or chronic wounds compromise the skin barrier.
Diagnosis For Skin Infections
Diagnosing a skin infection typically begins with a clinical examination and patient history. In some cases, doctors use lab tests like swabs, cultures, or skin scrapings to identify the exact pathogen and tailor treatment.
- Clinical Examination: Observation of redness, swelling, or rash.
- Skin Culture: Sample of fluid or tissue identifies bacteria or fungi.
- Skin Scraping: Microscopic examination for fungal elements.
- Biopsy: Small skin sample analyzed for unclear cases.
When To Seek Emergency Care For Skin Infections
While many skin infections are treatable in outpatient settings, some signs indicate serious complications or rapidly progressing disease that require immediate emergency evaluation.
If you notice the following, seek urgent care:
- Rapidly Spreading Redness: A sudden expansion of redness may indicate a fast‑spreading infection.
- High Fever or Chills: Could signal that the infection is affecting your whole body (systemic infection).
- Severe Pain Out of Proportion: Pain that feels much worse than expected may indicate deep tissue involvement.
- Pus With Foul Odor or Necrosis: Thick pus or tissue death requires immediate medical attention.
- Confusion or Lethargy: May be a sign of sepsis or a severe, serious infection.
Contact Exceptional Emergency Centers if symptoms are severe or worsening quickly.
Treatment For Skin Infections
Treatment depends on the type and severity. Mild infections may require topical creams, while severe cases may need systemic therapy. Treatments should always follow medical guidance.
1. Antibiotics (Doctor‑Recommended)
Doctor-recommended antibiotics like cephalexin or dicloxacillin eliminate bacteria and prevent spread. Completing the full course ensures recovery and reduces complications. Patients should follow their doctor’s instructions carefully and report any side effects, as improper use can lead to antibiotic resistance.
2. Topical Antifungals (Doctor‑Recommended)
Mild to moderate fungal infections, such as athlete’s foot or ringworm, respond to topical antifungals like terbinafine or clotrimazole, relieving itching and scaling while preventing spread. Consistent application for the full recommended duration is essential to prevent recurrence and fully eradicate the infection.
3. Oral Antifungals (Doctor‑Recommended)
Severe fungal infections may require oral antifungals such as fluconazole to treat systemic infection, speed recovery, and prevent recurrence. Doctors often monitor liver function during treatment to ensure safety, especially for prolonged courses.
4. Antiviral Therapy (Doctor‑Recommended)
For viral infections like shingles or herpes simplex, antivirals such as acyclovir reduce viral replication, shorten duration, and limit complications. Starting treatment early, ideally within 72 hours of symptom onset, maximizes effectiveness and helps prevent nerve-related pain.
5. Wound Care And Hygiene
Proper wound cleaning, drying, and covering reduce risk of secondary infections, support healing, and enhance effectiveness of prescribed medications. Regularly changing dressings and monitoring for signs of worsening infection ensures timely medical intervention if needed.
Exceptional Emergency Centers for Skin Infections
Skin infections can progress rapidly, especially if left untreated, and may require prompt medical attention. At Exceptional Emergency Centers, our skilled team provides quick evaluation and treatment in a fully equipped emergency setting. Early care can prevent complications like cellulitis, abscesses, or systemic infections.
With locations in Livingston, Beaumont, and Tyler, Exceptional Emergency Centers are ready to manage skin infections 24/7. Whether it’s redness, swelling, or painful lesions, our compassionate staff ensures patients receive timely care, helping them heal safely and comfortably. Quick action is essential when dealing with serious skin infections.